Degenerative Arthritis of the Knee | Osteoarthritis of the Knee
Osteoarthritis of the knee joint is one of the common forms of arthritis that damages the cartilage of the knee joint. Osteoarthritis silently develops and progresses through stages and thus takes several years to develop into fully blown osteoarthritis.
The symptoms in the initial stages are often mild as the disease progresses slowly. The stage four symptoms are severe causing damage to the cartilage, bone, and synovium of the knee joint. In almost all cases, the fourth stage of osteoarthritis requires surgery.
Cartilage supports the knee joint like a cushion and shock absorber
The cartilage of the knee joint works just like a cushion and a shock absorber. In other words, the knee joint is well-supported by natural cushioning in the form of cartilage. The knee joint has a Synovium – a soft tissue that produces synovial fluid for lubrication. As long as the cartilage is healthy, the joint remains healthy and the movement is smooth.
Osteoarthritis Induced Damage is Progressive
Osteoarthritis of the knee joint meaning: The damage to the knee joint happens gradually and the bones of the knee joint come very close to one another due to loss of the cartilage in between. In this scenario, bones rub against one another as the shock-absorbing capacity of the knee joint is lost due to excessive wear and tear of the cartilage. Those who suffer from this condition experience stiffness in the knee joint, pain, swelling, a feeling of warmth on the touch, walking difficulty. Therefore, osteoarthritis is commonly known as wear-and-tear arthritis.
The progression of osteoarthritis is gradual, silent, and may take several years to cause substantial damage to the knee joint. Symptoms may not manifest until osteoarthritis reaches advanced stages. The gradual and progressive damage occurs in stages – one to fourth as given below:
Stage 1
The damage caused to the cartilage is slight and the gap between the bones appears normal as there is no apparent narrowing of the space.
Individuals having osteoarthritis do not experience any symptoms during this stage.
Stage 2
This stage of osteoarthritis shows mild and minor damage to the knee joint. Though the space between the bones still appears normal, the affected area shows a hardening layer of the cartilage with thickened and dense areas. The affected person may experience joint stiffness, pain, and discomfort – especially after sitting for an extended period of time.
Stage 3
Cartilage progressively deteriorates becoming thin and worn out. The breakdown of the cartilage leads to narrowing of the gap between the bones – which can be seen in X-rays. The affected knee joint area starts paining and causes discomfort. Daily activities – such as walking, bending, and moving upstairs and downstairs become difficult. Synovial fluid builds up (synovitis) showing up joint inflammation. The person having this condition may feel the warmth on touch in the inflamed area of the knee joint.
Stage 4
This is the most advanced stage of OA, and the symptoms are quite apparent. The space between the bones in the joint has continued to narrow, causing the cartilage to break down further.
When this happens, there is stiffness in the joint, constant inflammation, and less fluid around the joint. There is more friction in the joint and more significant pain and discomfort while moving.
Osteoarthritis of the knee radiology
X-rays reveals bone on bone condition wherein either a very little cartilage left or the cartilage has completely worn out.
Those who develop this condition have bone lumps and feel the pain that augments with activities – such as walking.
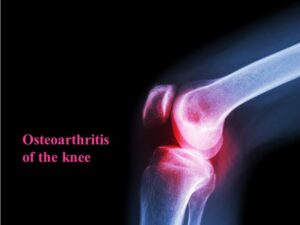
In severe cases, the bones may become deformed and angulated because of asymmetric loss of cartilage.
At this stage, surgical treatment remains the only option.
Causes of osteoarthritis of the knee joint
Age – The Major Risk Factor
Osteoarthritis of the knee is commonly seen in elderly people. In fact, advancing age is the most common risk factor for arthritis. Some degree of osteoarthritis develops in almost everyone who is aging.
though age is a major risk factor, young people can get it too. The risk of developing osteoarthritis increases after age 45. It can also be due to family history or hereditary; obesity, excessive wear and tear of the knee joint due to heavy physical activities;
Individuals involved in jobs that demand lots of activity including lifting heavy weights, squatting, kneeling, and moving up and downstairs are at increased risk of developing osteoarthritis of the knee owing to lots of pressure and stress on the knee joint.
Excess Body Weight
Excess weight on the knee joints due to obesity increases the risk of osteoarthritis many folds as obesity puts excess weight on all joints of the body especially the knee joints. Osteoarthritis is common in women than men as the risk in women increases after age 50 and above.
High-impact games and Heavy Physical Activities
Heavy physical activities increase the risk of wear and tear of the knee joint. Owing to this reason, people who play soccer, tennis and run long distances are at risk of developing osteoarthritis due to injury. On the contrary, moderate regular exercise is actually good for knee and joint health as it strengthens knee joints and decreases the risk of osteoarthritis.
Other illnesses
Individuals with some hormonal, autoimmune (rheumatoid arthritis), and growth disorders are more likely to develop osteoarthritis. In fact, rheumatoid arthritis is the second leading cause of arthritis. Individuals suffering from metabolic disorders such as iron overload or secretion of excess growth hormone in their bodies may have a higher risk of osteoarthritis.
Osteoarthritis of the knee Symptoms
- Pain, which is progressive
- Knee pain increases with activity but makes you feel better with rest
- Swelling of the knee joint
- Feeling of warmth in the knee joint
- Less mobility
- Stiffness in the knee joint (morning stiffness)
- Reduced knee mobility
- Difficulty in getting in and out of the car, chair, bed
- Difficulty walking on stairs
- Cracking sound in the knee with movement
Diagnosis
The orthopedic surgeon examines the patient carefully by taking into consideration all the signs and symptoms the patient is experiencing including the severity, location, and extent of pain. The doctor will also ask about the activities that are making the pain worse and whether resting is relieving the pain.
The doctor may also ask whether any other family member has a similar problem to determine if arthritis or any other issue is responsible for the pain. The doctor may order X- rays, blood tests, and other imaging tests to confirm the diagnosis of osteoarthritis and rule out other conditions like rheumatoid arthritis.
Osteoarthritis of the Knee Treatment Options
The main objective of osteoarthritis of the knee joint treatment is to relieve pain and improve mobility. To ensure this, an orthopedic surgeon provides treatment which is based on the stage of osteoarthritis and the damage caused to the knee joint.
In the initial stages, the treatment can include medications, lifestyle modifications, exercises, and physiotherapy sessions for improving bones and muscles strength and mobility.
First-stage Osteoarthritis of the knee joint Treatment
First stage osteoarthritis is usually asymptomatic. Even if the symptoms manifest, they are mild and can be relieved by taking over-the-counter (OTC) and other pain-relieving medications. Physiotherapy is also helpful in building the strength and mobility of bones. Though supplements may be recommended, there is no conclusive evidence to show that supplements can help.
Second-stage Osteoarthritis Treatment
The pain associated with stage 2 osteoarthritis is relieved by taking pain relievers. Flexibility, strength, the endurance of bones, cartilage, and muscles can be improved by physical therapy sessions. Lifestyle changes, minimizing high-impact activities, and avoiding weight-bearing activities can help avoid pain and minimize the damage.
Third and Fourth-stage Osteoarthritis Treatment
When the osteoarthritis progressively leads to the third and the fourth stages, the damage caused to the knee joint becomes significant – owing to which knee replacement surgery remains the only and the best option for the patient.
Total knee replacement is considered for those who have a severe knee injury or severe arthritis. Patients with osteoarthritis and impaired knee function or decreasing daily knee function, chronic pain, inflammation, swelling, stiffness and progressively increasing pain are the candidates for total knee replacement.


Recent Comments